FlossPoint: How Directional Shear During Movement Changes Recovery and Rehabilitation Outcomes
- Kyle Bowling

- 5 days ago
- 9 min read
Tissue flossing — the application of elastic compression bands during active movement — has been a standard tool in athletic training rooms and rehabilitation clinics for over a decade. The evidence base supporting its use for improving range of motion, joint mobility, and movement quality is well-established. What has been less well-defined is why some presentations respond immediately and durably, while others produce only temporary improvement before the restriction returns.
The answer lies in the mechanical specificity of the intervention. Uniform circumferential compression during movement produces diffuse shear across the entire wrapped segment. For restrictions localized to specific tissue interfaces under load, diffuse shear is a broad solution to a precise problem.
FlossPoint was developed over seven years of clinical work with collegiate and post-collegiate athletes to address this specificity gap. This article covers the mechanism, the evidence base it builds on, and the clinical application protocols that have produced the most consistent outcomes across lower extremity load-dependent restrictions.

The Mechanism: Focal Compression and Directional Shear
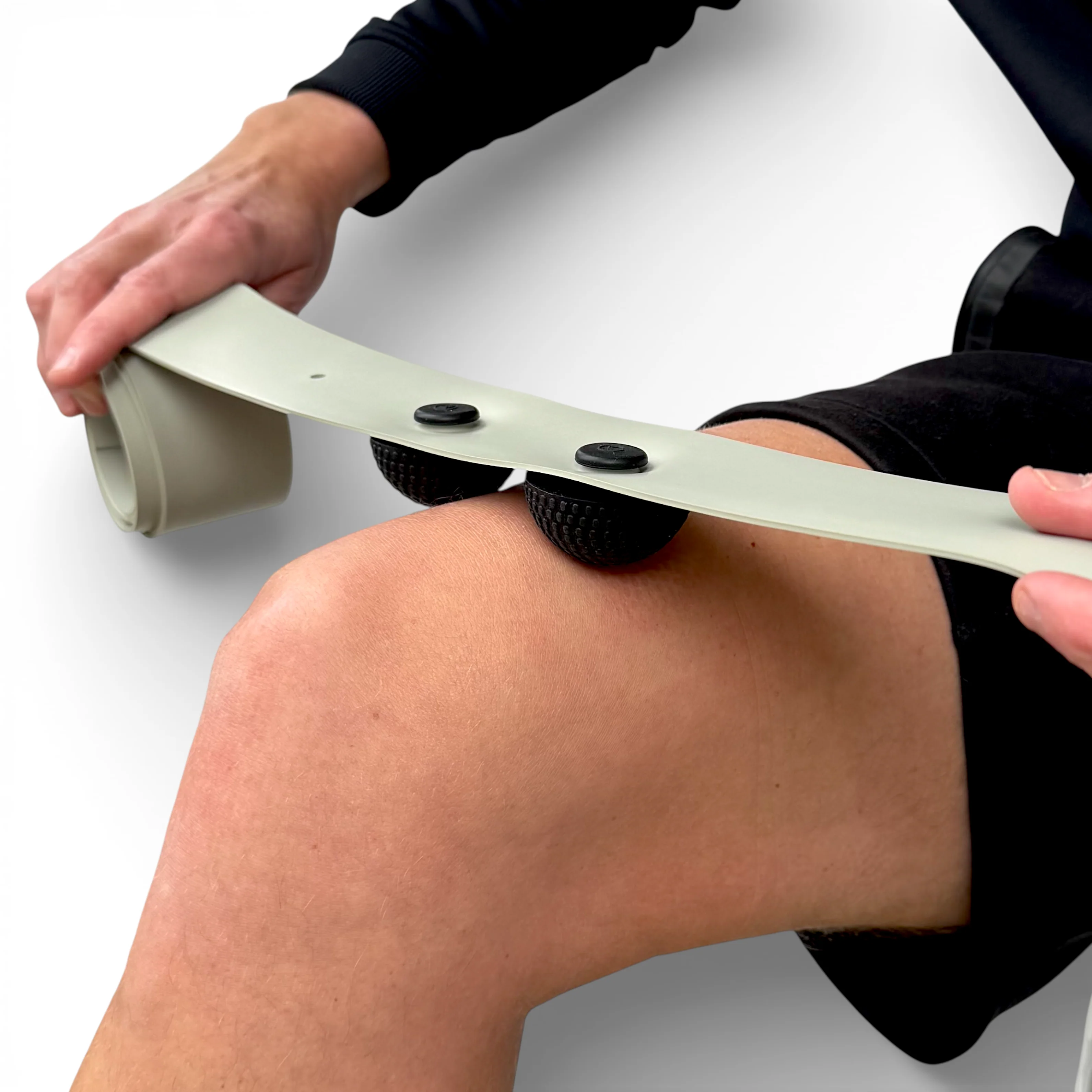
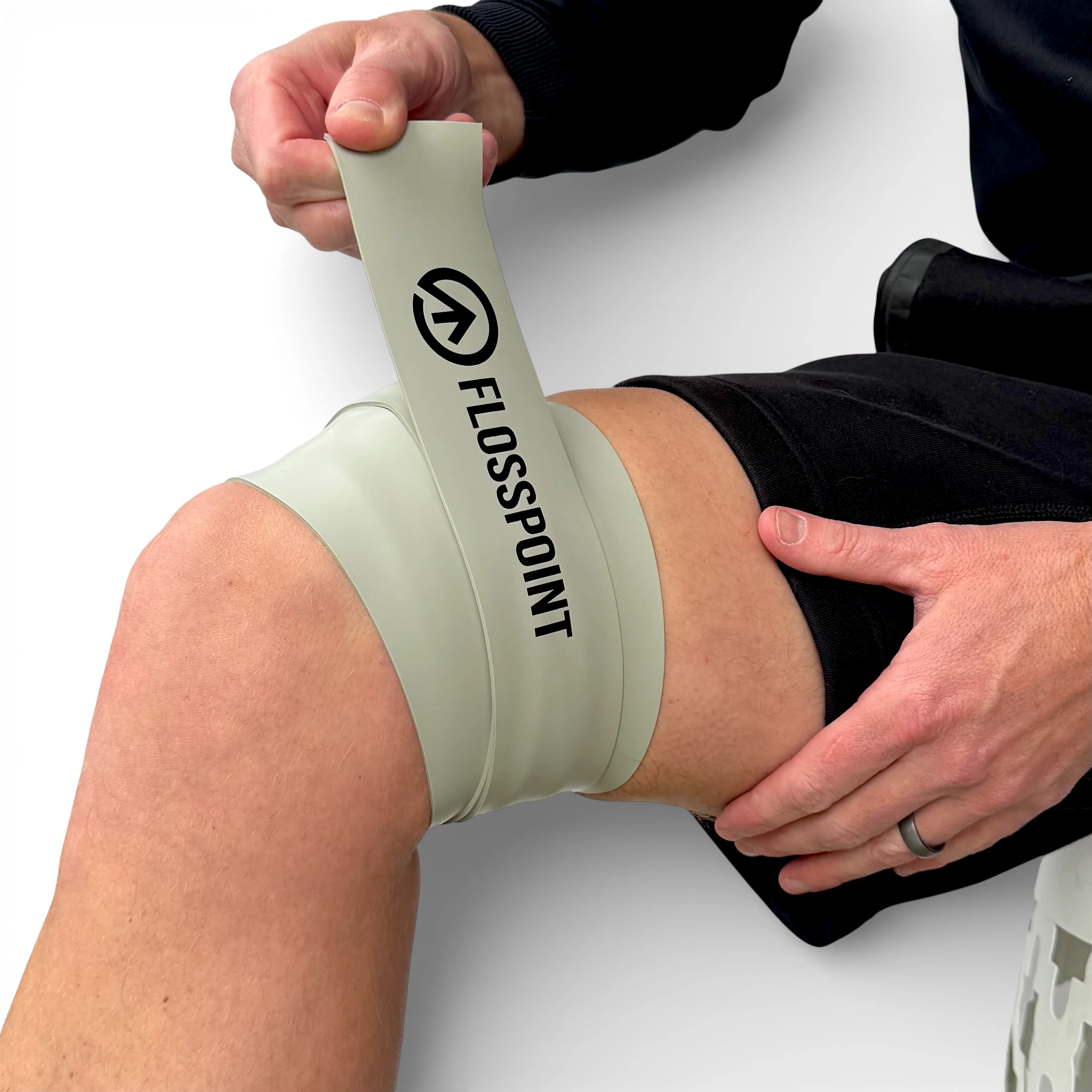
FlossPoint consists of a natural latex compression band and three removable ShearPoints — dome-shaped rubber grips that attach directly to the band and create focal compression at specific tissue interfaces rather than distributing pressure evenly across the wrapped segment.
The mechanical distinction is meaningful. When a standard floss band is applied, compression is distributed uniformly across the entire contact area. Tissue flattens evenly. During movement, shear forces are generated across the full width of the wrap — diffuse, non-specific, and not targeted to the precise interface where restriction is concentrated.
When ShearPoints are positioned at a specific tissue interface and the band is applied over them, compression is concentrated at 1-3 focal points. During movement, directional shear forces are generated at those specific points — parallel to the tissue surface, at the exact interface where sliding mechanics need to be restored.
Under MSK ultrasound, the difference is visible in real time. Standard compression flattens tissue layers together uniformly. Focal compression via ShearPoints during movement produces observable lateral movement between tissue layers at the targeted interface — the directional shear that challenges those interfaces to restore their sliding capacity under load.
Evidence Base
FlossPoint's mechanism builds directly on the established evidence for floss band compression during movement. The relevant literature supports several contributing mechanisms:
Fascial shearing: Compressed tissue interfaces are forced to move relative to each other during active movement, restoring sliding surface mechanics that may have been compromised by previous injury, accumulated training stress, or repetitive loading in restricted patterns.
The floss band generates significant mechanical compression around a muscle, retaining heat produced by elevated intramuscular pressure; it is hypothesized that this thermal and mechanical energy decreases the viscoelastic properties of the fascia — a property known as thixotropy — ultimately allowing for improved tissue elongation and interfascial glide (Konrad, Mocnik, and Nakamura, 2021; Daneshmandi et al., 2025).
Blood flow occlusion and reperfusion: Circumferential compression partially restricts blood flow to the wrapped segment. On removal, blood rushes back into the tissue — a reperfusion effect with proposed benefits for tissue recovery and tolerance. Researchers have postulated that vascular occlusion from the band stretch pressure, or the physiological cascade triggered on band release, may enhance hormonal responses and overall neuromuscular function. It has further been theorized that this form of ischemic preconditioning may increase tissue resistance to ischemia and its negative effects (Cheatham and Baker, 2024; Oliva-Lozano et al., 2024).
Neurophysiological changes: Compressive input alters how the nervous system processes sensation in the wrapped area, potentially reducing protective tension and allowing greater range under load immediately following application. Circumferential pressure applied by the floss band stretches the skin and underlying tissue, stimulating cutaneous and muscle mechanoreceptors, thereby modulating sensory feedback and altering the perception of stretch or discomfort. Evidence indicates that acute ROM gains following flossing are most consistent with increases in stretch tolerance or pain threshold rather than reductions in passive tissue stiffness — a neurophysiological mechanism also documented via decreased soleus H-reflex activity following floss band application (Kaneda et al., 2020; Cheatham and Baker, 2024).
Joint mobilization: When applied over a joint, circumferential compression modifies joint surface mechanics during active movement, addressing capsular restriction independent of soft tissue changes. Research comparing floss band application at the ankle joint versus calf soft tissue has documented short-term improvements in active and passive dorsiflexion ROM, jump performance, and dynamic balance — outcomes consistent with a direct joint-surface mechanical effect. Studies specifically wrapping the joint (rather than the soft tissue above it) have reported the most consistent changes in weight-bearing lunge test performance, suggesting that joint capsule mechanics are independently addressed by circumferential compression during loaded movement (Moon and Kim, 2022; Driller and Overmayer, 2017).
The consistent finding across the literature is that movement under compression is essential. Passive wrapping without active loaded movement produces substantially weaker outcomes. This is mechanistically coherent with the focal shear model: compression creates the conditions, movement generates the forces at the targeted interfaces.
Clinical Application: Lower Extremity Protocols
The following protocols represent the applications where directional shear during loaded movement has produced the most consistent and durable outcomes across seven years of clinical use with collegiate athletes.
1) Ankle Dorsiflexion Restriction
Ankle dorsiflexion restriction during loaded squatting or lunging — particularly when passive dorsiflexion range appears adequate — is one of the most responsive presentations to focal compression with movement.
Assessment: Weight-bearing lunge test or goblet squat. Identify whether the restriction is posterior (calf and Achilles complex) or anterior (tibialis anterior and anterior compartment). ShearPoint placement follows the restriction, not a standard template.
Posterior restriction: 2 ShearPoints positioned along the calf muscle belly, mid-point to lower third. Wrap from lower calf upward. Move through weighted heel-elevated split squats, slow goblet squats driving the knee forward over the toes, and walking for 2 minutes.
Anterior compartment restriction: 1-2 ShearPoints across the tibialis anterior, above the ankle joint. Wrap from the ankle upward across the shin. Move through the same loaded dorsiflexion patterns.
Reassessment: Remove the band immediately and retest the weight-bearing lunge. Improvement that holds under full training load confirms tissue tolerance was the limiting factor.
2) Calf and Achilles Complex Restriction
Load-dependent restriction in the calf and Achilles complex — presenting as tightness during push-off or eccentric loading rather than at rest — is the application where the original clinical observations behind FlossPoint were made.

ShearPoint placement: 2-3 ShearPoints along the calf muscle belly. For Achilles-proximal restriction, position the most distal ShearPoint at the musculotendinous junction. Avoid direct placement on the Achilles tendon itself.
Movement protocol: Loaded calf raises — slow eccentric emphasis — walking, and light jogging where appropriate. 2-3 minutes. The loaded push-off pattern is the target demand; the movement protocol should replicate it as closely as possible.
Key clinical indicator: Athletes with chronic calf restriction that survives foam rolling and stretching almost universally respond to this protocol. The restriction persisting through standard interventions is consistent with a load tolerance problem at the tissue interface rather than a length or general compliance problem.
3) Hamstring Restriction During Hip Hinge
The athlete with full passive straight leg raise who presents with proximal hamstring restriction during loaded Romanian deadlifts or good mornings represents one of the clearest examples of the passive range versus load tolerance distinction.
ShearPoint placement: 3 ShearPoints across the proximal to mid hamstring belly. For mid-belly restriction, distribute evenly across the restriction area. Avoid direct placement at the ischial tuberosity.
Movement protocol: Romanian deadlifts at light to moderate load, good mornings, and kettlebell swings with deliberate eccentric control. 2-3 minutes. The hip hinge under load is the target demand — replicate it during the protocol.
Athletes with previous hamstring strain: This is a particularly responsive population. Scar tissue and fascial adhesions at the injury interface can maintain load tolerance deficits long after passive range returns to normal. Targeting the previous injury site with focal compression during loaded hip hinge movement consistently produces meaningful improvement in this presentation.
4) Knee and Quadriceps Restriction
Anterior thigh restriction during loaded knee flexion — presenting during squats, step-ups, split squats, and terminal knee extension — responds to focal compression across the distal quadriceps.
ShearPoint placement: 2-3 ShearPoints across the distal quadriceps, above the patella. For lateral knee restriction, position ShearPoints along the IT band and lateral retinaculum. Avoid direct placement over the patellar tendon.
Movement protocol: Step-ups, split squats, and terminal knee extensions for anterior restriction. Lateral lunges and step-downs for lateral restriction. 2-3 minutes through the range that is restricted under load.
Contraindication: Acute inflammation, effusion, or confirmed pathology in the acute phase. This protocol is appropriate for chronic, load-dependent tissue restrictions once acute pathology has been ruled out.
5) Plantar Region and Foot
Plantar restriction during push-off and single-leg loading — particularly in runners — benefits from a combined approach addressing both the calf and the plantar region directly.
Protocol sequence: Address the calf first (2 ShearPoints, calf belly, 2 minutes). Reduced mechanical load transfer to the plantar fascia during push-off is often more impactful than direct plantar application alone. Follow with 1-2 ShearPoints across the midfoot if direct plantar restriction is present. Move through toe yoga, short foot activation, and single-leg balance with progressive loading.
Important note: This protocol is appropriate for load-dependent plantar restriction in the absence of acute inflammation. Significant heel insertion pain at rest, or presentations consistent with degenerative fasciopathy, require clinical assessment before applying load-based tissue work.
Protocol Principles
Across all applications, four principles govern consistent outcomes:
1. Load the movement first. Identify the restriction under the demand that reveals it — not at rest. This determines ShearPoint placement and the movement protocol. The restriction tells you where to put it.
2. Position at the tissue interface, not at the pain location. Pain location tells you where tissue is reporting distress. Movement assessment under load tells you where tissue is failing mechanically. These are often different.
3. Move with deliberate tempo. Two to three minutes of controlled movement through the restricted range under focal compression. Tempo matters more than speed. The goal is sustained mechanical input at the target interface under load — not rapid movement that minimizes time under tension.
4. Reassess under actual training load. The test is the movement that was restricted at the load that revealed the restriction. Passive range of motion testing after removal is insufficient. If the range holds under training demand, tissue tolerance improved. That is the only meaningful outcome measure.
Integration Into Clinical and High-Performance Practice
FlossPoint integrates into clinical and high-performance settings as a pre-training tissue preparation tool, a within-session adjunct to loading protocols, and a clinical manual therapy complement:
Pre-training application: 2-3 minutes per restricted area before training sessions where that restriction is a limiting factor. The improvement in tissue tolerance typically holds through the session when applied immediately before the demand.
Within loading protocols: Applied during warm-up sets of the restricted movement pattern. The athlete performs the loaded movement with the band on for the first 2-3 sets, removes it, and continues training. This approach integrates the tissue work directly into the training demand rather than treating it as a separate intervention.
Clinical adjunct: In rehabilitation settings, FlossPoint can be used as a dynamic pin-and-stretch tool during clinical sessions — the same mechanical principle as manual therapy compression with movement, but scalable across multiple applications and patient-led after initial instruction.
The learning curve for correct application is low. Most athletes and clinicians find consistent results within 2-3 applications once the placement logic — load the movement, identify the interface, position there — is understood.
Conclusion
FlossPoint is not a passive recovery tool. It does not work at rest. It works during the movement that reveals the restriction, at the tissue interface where that restriction lives, by generating the directional shear forces that challenge those interfaces to restore their sliding mechanics under load.
Seven years of clinical use with collegiate and post-collegiate athletes across multiple sports has produced a consistent finding: load-dependent tissue restrictions that do not respond to compression at rest respond to directional shear during loaded movement. The mechanism is accessible, the protocol is straightforward, and the outcome measure — does the range hold under training load — is unambiguous.
For restrictions that show up during movement, the intervention belongs during movement.
References
Cheatham, S. W. and Baker, R. (2024) 'Tissue Flossing: A Commentary on Clinical Practice Recommendations', International Journal of Sports Physical Therapy, 19(4), pp. 477-489.
Daneshmandi, H., Alghosi, M., Alimoradi, M., Monfaredian, O., Barati, A. and Granacher, U. (2025) 'Acute effects of tissue flossing on ankle range of motion in athletes with limited ankle dorsiflexion: a randomized controlled trial', BMC Sports Science, Medicine and Rehabilitation, 17:375.
Driller, M. W. and Overmayer, R. G. (2017) 'The effects of tissue flossing on ankle range of motion and jump performance', Physical Therapy in Sport, 25, pp. 20-24.
Kaneda, H., Takahira, N., Tsuda, K., Tozaki, K., Kudo, S., Takahashi, Y., Sasaki, S. and Kenmoku, T. (2020) 'Effects of Tissue Flossing and Dynamic Stretching on Hamstring Muscles Function', Journal of Sports Science & Medicine, 19, pp. 681-689.
Konrad, A., Mocnik, R. and Nakamura, M. (2021) 'Effects of tissue flossing on the healthy and impaired musculoskeletal system: a scoping review', Frontiers in Physiology, 12:666129.
Moon, B. H. and Kim, J. W. (2022) 'Effects of Floss Bands on Ankle Joint Range of Motion and Balance Ability', Physical Therapy Korea, 29(4), pp. 274-281.
Oliva-Lozano, J. M., Patterson, S. D., Chiampas, G., Maybury, E. and Cost, R. (2024) 'Blood flow restriction as a post-exercise recovery strategy: A systematic review of the current status of the literature', Biology of Sport, 41(3), pp. 191-200.

Dr. Kyle Bowling, DC is the Team Chiropractor for University of Kentucky Athletics and the Founder of Kentucky Sports Clinic and FlossPoint, a movement-based tissue loading system. FlossPoint was developed from seven years of clinical application with collegiate and post-collegiate athletes and uses removable ShearPoints to generate directional shear at tissue interfaces during loaded movement.




Comments