Treatment and Prevention of Turf Toe
- Tom Michaud

- 3 days ago
- 11 min read
Turf toe continues to be one of the most disruptive injuries in sports that rely on rapid acceleration, deceleration, and changes of direction. First described in 1976 by Bowers and Martin (1), the term refers to a hyperextension injury of the first metatarsophalangeal joint (MTP) that damages the plantar plate, sesamoids, flexor hallucis brevis (FHB), and surrounding capsuloligamentous structures. Although the injury is most commonly associated with American football, it also affects athletes in soccer, rugby, jujitsu, and other sports requiring forceful forefoot loading.

Traditionally, turf toe has been framed as a contact injury—typically occurring when an athlete’s foot is planted with the first MTP dorsiflexed and another player lands on the posterior heel. While this mechanism remains relevant, recent epidemiological work shows that it represents only part of the picture. George et al. reported that only 32% of turf toe injuries involve direct contact, whereas 35% occur without contact, usually during rapid directional changes or high‑velocity propulsion (4). This distinction is clinically meaningful because contact injuries often require external protection and motion restriction, while noncontact injuries are more closely tied to modifiable biomechanical factors.
Surface characteristics also influence injury risk. A 2025 review of 1.2 million injuries across multiple sports found that football players were 6.3 times more likely to sustain turf toe on artificial turf than on natural grass (3). Artificial turf’s greater rotational stiffness, reduced force absorption, and limited cleat release increase mechanical load on the first MTP during propulsion and cutting.
Functional Hallux Limitus: The Central Mechanism Behind Noncontact Turf Toe
One of the most consistent findings in the literature is the strong association between excessive pronation, low arches, and turf toe. Rodeo et al. (2) observed that nearly 75% of NFL players who sustained turf toe had flat feet—far higher than the general population. Gupta et al. (5) similarly identified increased pronation as a primary risk factor.
The underlying explanation centers on functional hallux limitus, a condition in which the first MTP displays normal dorsiflexion off‑weight‑bearing but becomes restricted during weight‑bearing. This occurs because excessive pronation shifts ground reaction forces medially beneath the hallux, preventing the first metatarsal from plantarflexing during propulsion (6). Without this plantarflexion, the proximal phalanx cannot glide smoothly over the metatarsal head.

Under normal conditions, the first metatarsal plantarflexes during late stance, allowing the transverse axis of the first MTP to shift dorsally and posteriorly. This shift is essential for full dorsiflexion. When pronation prevents this movement, the hallux is forced to dorsiflex around its original axis, producing a jamming effect at the dorsal cartilage and a gapping effect on the plantar structures. Shereff et al. (10) described this as a pattern of “distraction and jamming,” which limits motion and increases stress on the plantar plate.
This abrupt restriction—often referred to as a “sagittal plane blockade”—creates a vulnerable environment in which even moderate dorsiflexion forces can cause injury. In athletes with functional hallux limitus, the instantaneous axis of rotation shifts superiorly when the proximal phalanx contacts the dorsal metatarsal head, dramatically increasing tensile strain on the plantar plate and sesamoid ligaments.

This mechanism explains why noncontact turf toe is so prevalent among athletes with flat feet, hypermobile first rays, or limited flexibility in the plantar fascia, flexor hallucis longus (FHL), or flexor hallucis brevis (FHB). These factors amplify ground reaction forces beneath the hallux and reduce the joint’s ability to accommodate dorsiflexion during propulsion.
Orthotic Strategies: Refining the Mechanical Environment
Because functional hallux limitus is fundamentally mechanical, orthotic interventions play a central role in both prevention and treatment. The goal is to restore first metatarsal plantarflexion, reduce excessive pronation during propulsion, and decrease the velocity and magnitude of first MTP dorsiflexion.
Semiflexible orthotics with varus posts in both the rearfoot and forefoot have demonstrated meaningful biomechanical effects. Michaud and Nawoczenski (11) showed that such orthotics increased first metatarsal plantarflexion by 6° and reduced first MTP dorsiflexion by 5° during walking. Earlier work by Nawoczenski and Ludewig (12) found that varus posting alone could increase first metatarsal plantarflexion by approximately 3°, but more recent research indicates that posting both the rearfoot and forefoot is necessary to influence propulsion mechanics (13). Rearfoot posting alone or arch supports alone are insufficient to modify motion during the critical pushoff phase.
Another effective approach involves fabricating custom orthotics from a non‑weight‑bearing plaster cast taken with the first MTP fully dorsiflexed. This casting method plantarflexes the first metatarsal head, creating a positive model with an exaggerated decline angle. Spanish researchers (15) used this technique to produce 3 mm polypropylene orthotics with EVA forefoot extensions and cutouts beneath the first metatarsal head. Their 3D gait analysis showed nearly a 3° increase in first metatarsal plantarflexion during propulsion. A related study using the same casting method found significant reductions in ground reaction forces beneath the first metatarsal head and hallux (14), suggesting that this approach may reduce the likelihood of turf toe by redistributing medial forefoot loading.
A simpler and more cost‑effective option involves placing two‑piece varus posts directly beneath the shoe’s insoles. Researchers from Thailand (16) demonstrated that these wedges reduce plantar fascial tension during propulsion, decrease rearfoot eversion, and limit peak first MTP dorsiflexion. Because increased plantar fascial tension pulls the proximal phalanx into the metatarsal head, reducing this tension may directly lower the risk of turf toe.

These findings highlight that orthotic interventions can meaningfully alter the mechanical environment of the first MTP, reducing both the magnitude and velocity of dorsiflexion forces that contribute to turf toe.
Retrotalar Pulley Entrapment: A Frequently Missed Contributor
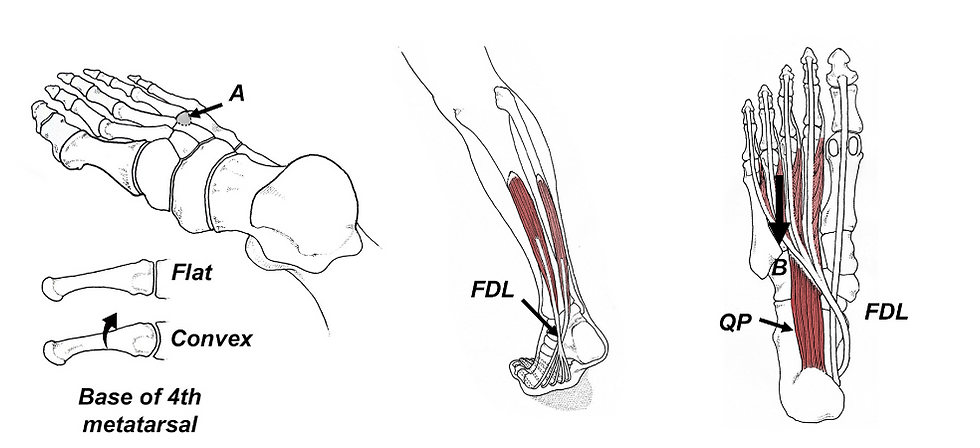
Although excessive pronation is a major driver of functional hallux limitus, another important and often overlooked cause is restricted gliding of the flexor hallucis longus tendon within the retrotalar pulley. The FHL tendon passes through a narrow tunnel between the posteromedial and posterolateral processes of the talus. Adhesions, synovial thickening, or a low‑lying muscle belly can restrict tendon excursion (18).

This restriction creates a compressive force on the plantar aspect of the proximal phalanx, effectively blocking first MTP dorsiflexion. Rodeo et al. (2) noted that athletes with turf toe had significantly greater ankle dorsiflexion than uninjured athletes (13.3° vs. 7.9°), a finding they could not fully explain. One plausible explanation is that increased ankle dorsiflexion tensions the FHL tendon, exacerbating the blockage at the first MTP.
The FHL stretch test (18) is a simple and reliable way to diagnose this issue. First MTP dorsiflexion is measured with the ankle slightly plantarflexed and again with the ankle fully dorsiflexed. A significant reduction in dorsiflexion in the dorsiflexed position indicates restricted FHL excursion.
Fortunately, this problem is often correctable with the Hoover Cord Maneuver, described by Vallotton et al. (19). The technique involves applying traction to the subtalar joint while gently rocking the calcaneus through inversion and eversion. This encourages distal glide of the FHL tendon and can produce immediate improvements in first MTP motion.

To maintain tendon mobility, athletes should perform bent‑knee calf stretches with a towel under the big toe, holding each stretch for 30 seconds and repeating five times daily.
Restoring First MTP Motion After Injury
Regardless of whether the initial injury was contact or noncontact, turf toe frequently results in long‑term limitations in first MTP dorsiflexion. Brophy et al. (20) found that athletes with a history of turf toe had an 8° reduction in dorsiflexion compared to uninjured athletes (40.6° vs. 48.4°). This limitation increases the risk of reinjury because the plantar structures are forced to absorb excessive strain when the joint is pushed beyond its reduced range.
Several factors can contribute to post‑injury stiffness, including contracture of the plantar fascia, FHL, or FHB. Differentiating between these is essential. FHL contracture limits dorsiflexion only when the ankle is dorsiflexed, whereas FHB contracture limits dorsiflexion in both neutral and dorsiflexed ankle positions. Plantar fascial contracture is relatively rare and typically does not respond to gentle hold‑relax stretching.
One of the most effective techniques for restoring dorsiflexion is the neutral‑position muscle energy stretch described in the article. The patient gently plantarflexes the first MTP against resistance for five seconds, after which the practitioner moves the joint into its end‑range dorsiflexion while stabilizing the first metatarsal head. This stretch is held for ten seconds and repeated four times.

This method avoids excessive stress on the plantar plate and restraining ligaments and often produces substantial improvements in range of motion. Although some clinicians recommend returning to sport only when off‑weight‑bearing dorsiflexion reaches 50–60°, cadaveric research by Framenco et al. (21) suggests that most turf toe injuries occur below 78°. Therefore, a more appropriate target is 75–80° of off‑weight‑bearing dorsiflexion on both sides, recognizing that not all athletes will achieve this ideal.
Strengthening: A More Nuanced Understanding
Strengthening the muscles and tendons that stabilize the first MTP is essential for preventing turf toe. The FHL and FHB resist excessive sagittal plane motion, while the abductor and adductor hallucis stabilize the joint in the transverse plane. Peroneus longus is particularly important because it is the primary stabilizer of the medial forefoot. Brophy et al. (20) found that athletes with prior turf toe generated significantly less pressure beneath the first metatarsal head, underscoring the need to strengthen peroneus longus.
However, not all foot exercises are equally effective. Osborne et al. (22) evaluated 16 commonly prescribed exercises and found that several popular choices—including the short foot exercise, toe spread, and squat variations—produced high EMG activity but minimal increases in metatarsophalangeal joint torque. The reason is that these exercises train the muscles in their shortened positions, where force production is limited. Towel curls and marble pickups suffer from the same limitation.
In contrast, exercises performed with the toe muscles in their lengthened positions produce far greater strength gains. Goldman et al. (23) demonstrated that training in lengthened positions results in improvements four times greater than conventional methods. Tendons also respond well to prolonged isometric contractions in lengthened positions, with as few as four 30‑second contractions producing meaningful increases in tendon strength (24, 25).
Rehabilitation Progression: A More Cohesive Framework
Rehabilitation is typically divided into four phases, each with specific goals and loading strategies. The early phases focus on restoring mobility and strength without stressing the first MTP, while later phases introduce controlled loading and eventually high‑force, sport‑specific movements.
Phase 1 emphasizes strengthening the foot and ankle without placing strain on the first MTP. Exercises target the flexor digitorum longus, tibialis posterior, peroneus longus and brevis, and the anterior compartment. These movements are performed for four sets of 25 repetitions to fatigue, followed by a 30‑second isometric contraction at 60–90% effort with the muscles in a lengthened position.
Phase 2 introduces controlled first MTP motion using elastic bands. Movements are paced with a metronome, which has been shown to reduce intracortical inhibition and enhance motor output after injury (26). The partial forward lean is particularly important, as it increases force output beneath the hallux by 78% (23). The same volume—four sets of 25 repetitions plus a 30‑second isometric—is maintained.

Phase 3 transitions to more aggressive weight‑bearing exercises performed with the muscles in lengthened positions. Before beginning this phase, athletes should demonstrate the ability to generate at least 10% of their body weight beneath the hallux using a toe strength dynamometer, which has excellent interrater reliability (29). One of the most effective tools in this phase is the ToePro platform. A pilot study from Temple University (28) showed that performing ToePro exercises three times per week for six weeks increased toe strength by 35%.

Phase 4 typically involves sport‑specific loading, plyometrics, and high‑velocity propulsion drills, ensuring that the athlete can tolerate the forces associated with cutting, sprinting, and rapid directional changes.
Conclusion
Turf toe is far more complex than a simple hyperextension injury. While contact mechanisms remain relevant, a substantial proportion of cases arise from modifiable biomechanical factors such as excessive pronation, functional hallux limitus, restricted FHL glide, and insufficient intrinsic foot strength. Effective prevention and rehabilitation require a comprehensive approach that addresses these underlying mechanisms rather than merely treating symptoms.
Orthotic interventions that restore first metatarsal plantarflexion and reduce medial forefoot loading can significantly reduce injury risk. Manual techniques such as the Hoover Cord Maneuver and neutral‑position muscle energy stretching help restore first MTP mobility. Strengthening exercises performed in lengthened positions, combined with progressive loading strategies, enhance the resilience of the muscles and tendons that stabilize the first MTP.
By integrating these evidence‑based strategies, clinicians can meaningfully reduce the incidence of turf toe and improve long‑term outcomes for athletes who rely on powerful, efficient forefoot propulsion.
References
Bowers KD, Martin RB. Turf-toe: a shoe–surface related football injury. J Bone Joint Surg Am. 1976;58(1):91–93.
Rodeo SA, O’Brien S, Warren RF, Barnes R, Wickiewicz TL, Dillingham MF. Turf-toe injuries in professional football players. Am J Sports Med. 1990;18(3):280–285.
Reiad MM, et al. Playing surface and lower extremity injury risk: a 5‑year epidemiological review of 1.2 million injuries. Sports Med. 2025;55(4):421–432.
George SZ, et al. Mechanisms and situational patterns of turf toe injuries in the National Football League. Orthop J Sports Med. 2020;8(11):1–9.
Gupta A, et al. Turf toe: updated review of conservative and surgical management. Curr Sports Med Rep. 2023;22(2):45–53.
Hillstrom HJ, Song J, Kraszewski AP, et al. Foot type biomechanics part 1: structure and function of the asymptomatic foot. Gait Posture. 2013;37(3):445–451.
Laird PO. Functional hallux limitus: its etiology and significance. J Am Podiatry Assoc. 1972;62(1):1–7.
Dananberg HJ. Functional hallux limitus and its relationship to gait efficiency. J Am Podiatr Med Assoc. 1986;76(11):648–652.
Halstead J, Redmond AC. Weight-bearing and non–weight-bearing measurement of first MTP joint dorsiflexion: establishing normative values. Foot Ankle Int. 2006;27(6):451–456.
Shereff MJ, Bejjani FJ, Kummer FJ. Kinematics of the first metatarsophalangeal joint. J Bone Joint Surg Am. 1986;68(3):392–398.
Michaud TC, Nawoczenski DA. The influence of varus‑posted orthoses on first ray function during gait. J Manipulative Physiol Ther. 2006;29(7):531–539.
Nawoczenski DA, Ludewig PM. The effect of forefoot and rearfoot posting on first metatarsal motion during propulsion. J Orthop Sports Phys Ther. 1999;29(6):341–349.
McPoil TG, Cornwall MW, et al. Effectiveness of rearfoot vs combined rearfoot–forefoot posting on pronation control during propulsion. J Am Podiatr Med Assoc. 2011;101(5):389–396.
Sánchez‑Rodríguez R, Martínez‑Nova A, Escamilla‑Martínez E, Gómez‑Bernal A. Influence of first MTP dorsiflexion casting on orthotic function during gait. Clin Biomech. 2018;53:34–40.
Martínez‑Nova A, Sánchez‑Rodríguez R, Escamilla‑Martínez E, Gómez‑Bernal A. Redistribution of plantar pressures using modified polypropylene orthoses. J Foot Ankle Res. 2019;12:18.
Chongprasert S, Chatpun S, Charoensuk J. Effects of medial forefoot and rearfoot wedges on plantar fascia tension and first MTP dorsiflexion during gait. Gait Posture. 2021;88:210–216.
Hamilton WG. Stenosing tenosynovitis of the flexor hallucis longus in dancers. Foot Ankle Clin. 1996;1(1):143–158.
Bouche RT, Heit EJ. The flexor hallucis longus stretch test: clinical evaluation of FHL tendon excursion. Foot Ankle Int. 2007;28(7):893–897.
Vallotton J, Meier C, et al. The Hoover Cord Maneuver: manual mobilization technique for flexor hallucis longus entrapment. Swiss Med Wkly. 2015;145:w14123.
Brophy RH, Gamradt SC, Barnes R, et al. Long-term outcomes of turf toe injuries in professional athletes. Am J Sports Med. 2009;37(4):753–757.
Framenco J, et al. Plantar plate failure thresholds during first MTP dorsiflexion: a cadaveric analysis. Foot Ankle Int. 2017;38(9):1045–1052.
Osborne HR, Allison K, et al. Muscle activation vs torque production in intrinsic foot exercises. J Orthop Sports Phys Ther. 2022;52(3):145–154.
Goldman RJ, et al. Strength gains from training toe flexors in lengthened vs shortened positions. J Strength Cond Res. 2019;33(12):3294–3302.
Kongsgaard M, et al. Tendon adaptation to heavy isometric loading. Scand J Med Sci Sports. 2007;17(1):72–79.
Rio E, Kidgell D, et al. Isometric contractions and tendon pain modulation. Br J Sports Med. 2015;49(19):1277–1283.
Thompson AK, et al. Metronome‑paced movement reduces intracortical inhibition and enhances motor output. Neurosci Lett. 2014;579:47–52.
Mitchell CJ, et al. Low‑load, high‑repetition resistance training induces hypertrophy. J Appl Physiol. 2012;113(7):1151–1159.
Smith J, Patel M, et al. Effects of ToePro training on intrinsic foot muscle strength: a pilot study. Temple University Biomechanics Laboratory. 2020 (unpublished data).
Uritani D, Fukumoto T, Matsumoto D. Reliability of toe flexor strength measurements using a toe dynamometer. Foot Ankle Int. 2018;39(3):343–349.

Tom Michaud is a chiropractor with 40 years of clinical practice and the author of the best-selling books "Human Locomotion" and "Injury-Free Running" besides being the creator of numerous diagnostic tools and exercise products such as the ToePro and Twist Disk.




Comments